Mental Health is Metabolic: What This New Consensus Means for Ketogenic Therapy
Ketogenic therapy is gaining traction in mental health care, and a new consensus paper helps bring structure to how it can actually be used in practice.
The recently published paper, “Awareness and Best Practices in Using Ketogenic Therapy to Treat Serious Mental Illness: A Modified Delphi Consensus,” brings together expert opinion on how ketogenic metabolic therapy (KMT) can be used in conditions like depression, bipolar disorder, and schizophrenia.
And while this isn’t a randomized controlled trial, it’s something arguably just as important at this stage: alignment among clinicians who are actually doing the work.
First — What is a Delphi Consensus (and Why Should We Care)?
A Delphi consensus is a structured way of gathering input from a group of experts and refining it over multiple rounds until a clear agreement emerges. Instead of debating in a room, experts respond independently to a series of statements, review summarized group feedback, and adjust their responses over time. This process helps reduce bias and builds thoughtful, experience-driven agreement.
In this case, a steering group of mental health and metabolic experts developed key statements that were then reviewed by 47 clinicians. Through this process, consensus was reached on how to safely and effectively use KMT in serious mental illness.
So why does this matter?
In areas where large clinical trials are still emerging, clinical experience often leads the way. A Delphi consensus helps bridge the gap between early research and real-world practice. It gives us insight into how experienced clinicians are thinking, what they are actually doing, and where the field is heading. This is very similar to how KMT evolved in epilepsy, and the same pattern is unfolding in mental health.
Why We Need Additional Tools in Serious Mental Illness
One important point highlighted in this paper is that innovation in psychiatric medications has been limited in recent years. We often cycle through medications with similar mechanisms, and for a subset of patients, particularly those with treatment-resistant conditions, outcomes do not meaningfully change.
This is where the parallel to epilepsy is hard to ignore.
In epilepsy:
Patients who do not respond to initial medications often remain refractory
Adding additional medications rarely changes that trajectory
In mental health, we see a similar pattern:
Treatment-resistant depression
Persistent bipolar symptoms
Chronic schizophrenia
This does not mean we are without options. It does highlight that for some patients, we may need to think beyond a medication-only approach.
So, the question becomes: are we ready to incorporate additional tools that target underlying physiology, not just symptoms?
Metabolic Link to Mental Health
One of the most compelling sections of this paper highlights the relationship between mental health and metabolic health.
Prediabetes: 2.7x higher risk of depression
Bipolar disorder: 3.5x higher rates of metabolic syndrome
Schizophrenia: 3.7x higher rates of insulin resistance
We know that insulin resistance is linked to impaired brain energy metabolism and improving metabolic health can improve psychiatric symptoms.
This is where KMT becomes incredibly relevant. Because at its core, KMT is not just a “diet.”
It’s a metabolic intervention.
What Did Experts Actually Agree On?
1. Ketogenic Metabolic Therapy Has a Role
There was 100% agreement that KMT shows promise in treating serious mental illness.
2. Who is a Good Candidate?
Experts strongly agreed KMT may be appropriate for:
Individuals with treatment-resistant conditions
Those who cannot tolerate medications
Those who prefer non-pharmacologic options
Individuals with metabolic dysfunction
Or simply those who want to try it
KMT is not a “last resort”, but rather a valid option within the spectrum of care.
3. This is NOT a Quick Fix
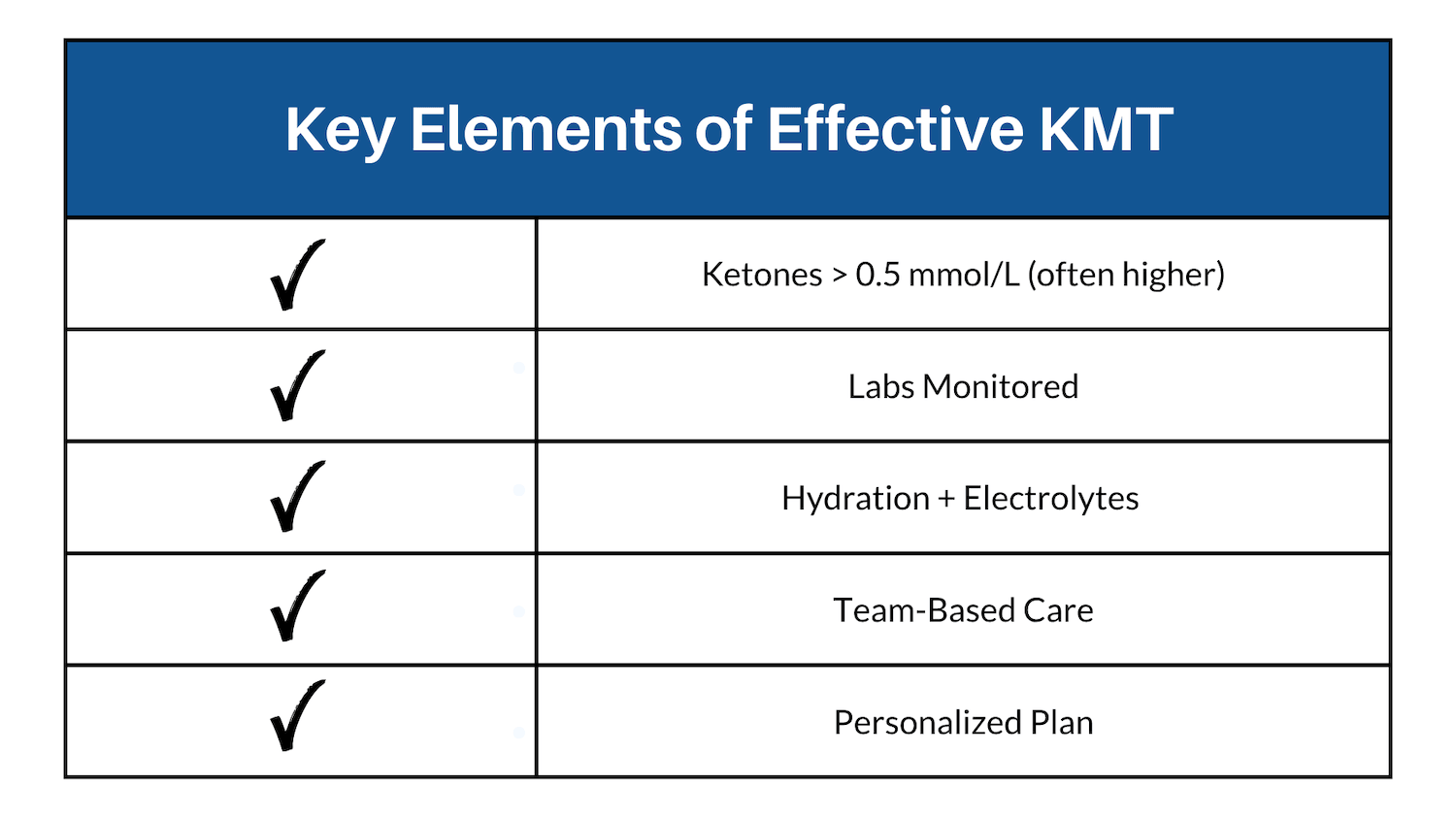
The paper highlights the importance of setting realistic expectations, with strong agreement among the expert panel. Ketosis typically begins around 0.5 mmol/L BHB, though many patients may need levels closer to or above 1.0 mmol/L for optimal outcomes. Just as important, benefits often take weeks to months and require consistent ketosis over time. This is not a quick fix, but a metabolic adaptation process that takes time.
4. Monitoring Matters
The consensus emphasized the importance of monitoring including regular ketone tracking, along with routine lab work such as complete blood count, metabolic panel, lipid panel, insulin, vitamin levels, and carnitine. Attention to hydration and electrolytes is also critical. In practice, this means KMT should not be implemented casually or without proper clinical guidance.
5. Clinical Support & Early Considerations
The consensus reinforces that KMT should be implemented with a trained clinical team, including nutrition professionals and prescribing providers. This goes far beyond simply changing diet. It involves medication adjustments, metabolic monitoring, and individualized nutrition planning.
An important nuance, especially in mental health, is that symptoms can temporarily worsen during early adaptation. Patients may experience mood changes, irritability, anxiety, or even short-term worsening of depression or psychosis. This makes education and close support essential to set expectations, guide patients through the transition, and prevent premature discontinuation.
Safety Still Comes First
The paper also outlines clear contraindications, including pregnancy, pancreatitis, liver failure, certain metabolic disorders, and situations requiring close medical oversight (to name a few). Importantly, KMT is not appropriate as a standalone treatment in acute or unstable psychiatric situations. It is not a replacement for urgent care, but rather a structured, longer-term therapeutic strategy.
So… Where Does This Leave Us?
This paper doesn’t give us all the answers. But it does give us something highly valuable including a way to:
Identify appropriate patients
Implement therapy safely
Monitor effectively
Set realistic expectations
And maybe most importantly, it validates what many clinicians and patients are already experiencing.
The AKT Perspective
At AKT, this is exactly the space we live in. We work with patients who have tried everything, families searching for a different path, and clinicians looking for better tools. This paper reinforces is that KMT is no longer fringe. It is becoming part of the clinical conversation, not as a replacement for everything else, but as a powerful, metabolically driven option.
If you are interested in exploring this further, feel free to read the full consensus statement, which is available online for free. It was written by leading experts in the field including Dr. Georgia Ede, Dr. Matthew Bernstein, Dr. Lori Calabrese, Dr. Iain Campbell, Nicole Laurent, Dr. Chris Palmer, Dr. Shebani Sethi, and Beth Zupec-Kania, RDN, CD. Beth is a registered dietitian, respected leader in ketogenic therapy with over 30 years of experience, and a close colleague whose work has helped shape this field .